Diabetes and Eye (Diabetic Retinopathy)
Diabetes is a disease that affects many organs of the body
like eyes, kidney, nervous system, heart, limbs etc.
Diabetes causes many changes in the eye. The most
significant vision threatening consequence of diabetes in
the eye is Diabetic Retinopathy and its complications.
Untreated, it may cause blindness. However, timely
diagnosis and proper management of this condition can
help the patients maintain a useful vision and lead a
socially productive life.
How does diabetes affect the eye?
Diabetes may lead to frequent fluctuations in vision and
change in glasses power. It may also lead to Cataract at a
younger age, Glaucoma, decreased vision due to
involvement of the optic nerve, temporary paralysis of the
eye muscles and thus double vision, Diabetic Retinopathy
etc.
What is Diabetic Retinopathy?
Retina is the innermost layer at the back of the eye. The
images of what we see are formed on this light sensitive
layer and are then transmitted to the brain by optic nerve.
Long standing Diabetes, causes some changes in the retina
and thus decreases the vision.
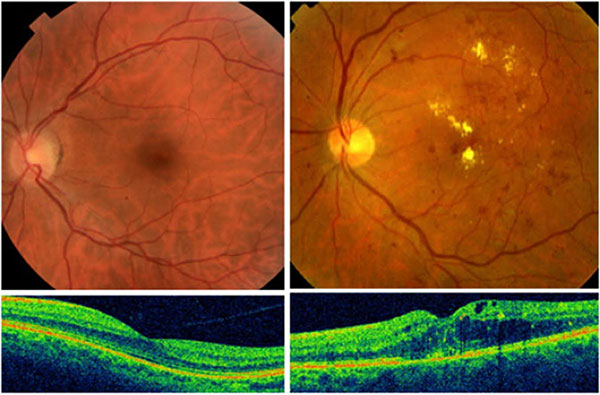
Initially the small vessels of the retina are affected. They
leak fluid and blood in the retina causing tiny hemorrhages
and swelling of the retina, and thus decrease vision. In the
later stages, the small blood vessels of retina close and lead
to formation of new blood vessels. These new vessels are
very fragile and bleed very easily to cause bleeding into the
eye (Vitreous Hemorrhage). This bleeding causes severe
vision loss, and many a times leads to secondary changes in
the retina and eye to damage it beyond repair.
What are the risk factors fordiabetic retinopathy?
Though any patient with diabetes may develop Diabetic
Retinopathy, the longer the person has diabetes, the greater
are his/her chances to develop Diabetic Retinopathy.
Majority of the patients who have had diabetes for more
than 5 years do have some changes of Diabetic Retinopathy.
The other risk factors are high blood pressure, anemia,
kidney diseases, and pregnancy.
Can we prevent Diabetic Retinopathy?
There is no treatment that can prevent Diabetic Retinopathy
altogether. But it has been proven that a good control of
diabetes can delay and slow down the rate of progress of
Diabetic Retinopathy and its complications. One must
exercise regularly, keep the blood pressure under control,
and avoid smoking.
Why is Early Detection important?
The vision lost due to Diabetic Retinopathy is not regained,
and the aim of the treatment is to preserve the vision and not
to improve the vision. In the earlier stages of the disease
when the vision is not affected, there may be no symptoms
perceived by the patient. It is best to detect the disease at this
early stage before significant vision loss has occurred, and
perform a timely treatment, as and when required. This
early detection can only be achieved by periodic evaluation
(every 6 months to 1 year) of the eyes of every diabetic
patient by an eye surgeon, preferably a retina specialist,
even if they have no eye related symptoms.
What is Fluorescein Angiography?
It is a test in which a series of photographs of the retina are
taken with the help of a special camera. These photographs
are taken after giving the patient an injection of a yellow
dye. This dye reaches the retina through the blood stream
and helps in evaluating the blood vessels of retina more
clearly. This test helps the doctor to determine which areas
are to be treated with laser. It is also done after laser
treatment to monitor the progress of disease and to
determine the need of further laser.
What is Optical Coherence Tomography (OCT)?
It is a test which gives a very high resolution cross sectional
image of the retina and also gives information about the
retinal thickening and the type of swelling of the retina. It is
very useful in deciding the treatment of Diabetic
Retinopathy and also for monitoring the follow-up of these
patients.
What is the Treatment for Diabetic Retinopathy?
The treatment required depends upon the stage of the
disease. In the very initial stages, just periodic follow ups are
advised to look for progression of disease. Laser treatment is
recommended when there is significant swelling in the
macula (maculopathy), or when there are significant new
blood vessels in the retina or iris. In certain cases, Intravitreal
anti-VEGF agents (Lucentis/Eylea/Avastin) or Steroids
(Ozurdex) are used along with laser and surgical treatment.
In advanced stages with Vitreous Hemorrhage, retinal
detachment etc., surgery (Vitrectomy) may be required.
What is Laser treatment?
Laser is a highly concentrated light that is beamed onto the
retina to treat the desired area. It is a painless OPD procedure
that does not require admission. It may require more than one
sitting to complete the treatment.
It is important to remember that the laser treatment is done to
prevent or retard further loss of vision and not to improve the
vision. It is highly effective, and a timely treatment can
prevent blindness in about 80% of the treated patients.
What are the Side Effects of Laser?
The laser treatment may have a few side effects like decrease
in the peripheral field of vision, decrease in color vision and
difficulty in seeing at night. Sometimes it may also reduce
the central vision. This is usually temporary but sometimes
this may not improve.
Though no treatment is without any side effects, the risks of
the laser treatment are far less than the risk of not having
the treatment.
What is anti VEGF treatment (Lucentis/Eylea/Avastin)
or Steroids Treatment (Ozurdex)?
These medicines are injected within the eye in a very small
dose. It helps in decreasing the swelling of the retina, helps
in controlling the new blood vessels and also makes the
subsequent Vitrectomy surgery easier. These injections have
improved the results of treatment of Diabetic Retinopathy
very significantly.
What Surgery is done for Diabetic Retinopathy?
In some patients in which the disease is not controlled by the
laser, or who have reached the advanced stage of disease,
Vitrectomy and additional surgical procedures may be
required. In Vitrectomy surgery, the retinal surgeon removes
the blood filled vitreous and replaces it with a fluid, using
very delicate instruments with the help of a microscope.
What are the newer developments in Vitreo Retinal Surgery?
With the ever improving experience and better machines, we
are able to reduce the time taken for the surgery and
maximizing the results and comfort for the patients. The
newer machines can help us perform surgeries through
smaller incisions MIVS (23 G, 25 G and 27 G) and can
achieve a fast cut rate (7500/min and more) to make the
surgery safer and faster.
Synergy Eye Care and its Doctors specialise in Advanced Retinal Care and is equipped with FA, OCT, Lasers, Latest Vitrectomy machines etc. to take care of patients with various stages of Diabetic Retinopathy and offers all forms of treatment like Injections, Lasers and Surgeries with good results.
Disclaimer: Information published here is for educational purposes only and is not intended to replace medical advice. If you suspect that you have a health problem, please consult your doctor immediately